CMS considering automatic enrollment in a Medicare Advantage plan
Two news reports last week that could impact EMS reimbursement should catch the attention of EMS leaders.
The first report signals that Medicare is considering making enrollment in Medicare Advantage (MA) the ‘default’ enrollment option.
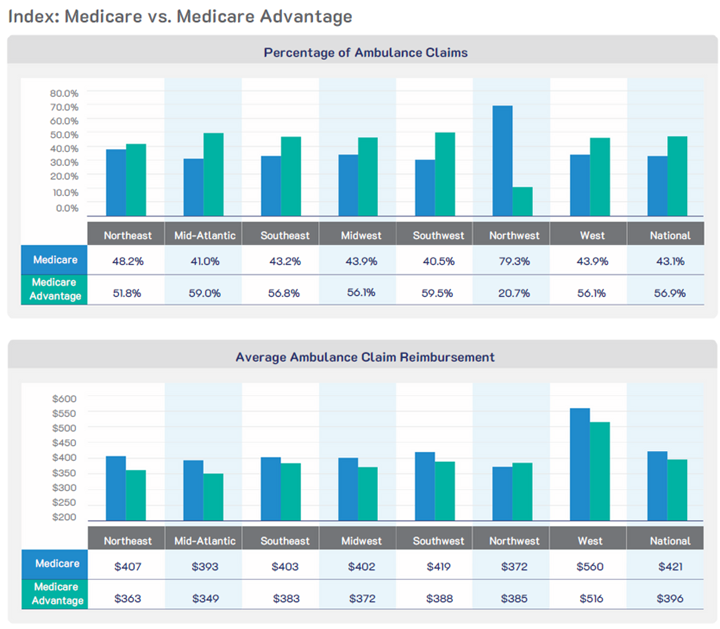
As reported in the August 2025 PWW|AG EMS Financial Index Report, MA claims represent 56.9% of all ambulance claims, with Medicare Part B representing 43.1% of claims. The average reimbursement from MA plans is $25 lower than Medicare Part B. Additional enrollees in MA plans could have a negative impact on EMS reimbursement.
The second report reveals that the average out-of-pocket premiums for Affordable Care Act (ACA) enrollees rose 58% this year after the expiration of enhanced subsidies. Also, 1.2 million fewer people enrolled in ACA plans in 2026 compared to 2025.
This possibility was discussed in our summer Pulse of EMS Finance webinar series, explaining that reduced ACA enrollment due to provisions contained in the OBBBA could shift commercially insured patients to uninsured, or Medicaid programs.
We strong encourage EMS leaders to closely monitor these types of developments, and consider modeling what these changes may mean for their revenue cycle.
—————
CMS considering automatic enrollment in a Medicare Advantage plan
The idea is part of the conservative Project 2025 policy.
By Susan Morse
March 24, 2026
The Centers for Medicare & Medicaid Services is considering a policy to automatically enroll seniors in a Medicare Advantage plan, according to STAT.
Chris Klomp, director of Medicare and deputy administrator for CMS, told STAT his team is mulling the feasibility of models that would either automatically enroll beneficiaries into a private Medicare Advantage plan or an accountable care organization that participates in the Medicare Shared Savings Program or similar program.
Klomp said either choice would be better than enrolling beneficiaries in a fee-for-service arrangement, which is Medicare. Individuals could still opt into a different insurance arrangement, he said.
Klomp is senior advisor to Health and Human Services Secretary Robert F. Kennedy, Jr.
In February, Kennedy announced in an email to staff that he was remaking his leadership team, putting Klomp in charge of overseeing all HHS operations, according to Politico.
Currently, original Medicare is the default option for seniors who don’t make a choice. Over half of seniors enrolled in a Medicare plan choose a Medicare Advantage plan.
Moving to MA as the default option is part of the conservative Project 2025 policy blueprint, which has made other recommendations that HHS has initiated such as Medicaid work requirements.
Medicare Advantage (MA), a system of competing private health plans, is the major alternative to traditional Medicare for America’s large and growing cohort of seniors. The program provides beneficiaries with a wide range of competitive health plan choices—a richer set of benefits than traditional Medicare provides and at a reasonable cost. Equally as important, the MA program has been registering consistently high marks for superior performance in delivering high-quality care. Critical reforms are still needed to strengthen and improve the program for the future.”
————
ACA premium costs up after subsidies expire
By Peter Sullivan
March 30, 2026
https://www.axios.com/newsletters/axios-vitals-f319f390-2b23-11f1-8489-774d2aecabb5.html
Average out-of-pocket premiums for Obamacare enrollees rose 58%, or $65 per month, this year after the expiration of enhanced subsidies, new federal data shows.
Why it matters: The data helps quantify the effects of the fierce partisan battle in Congress over whether to extend the subsidies, which ended in no action.
By the numbers: The average Affordable Care Act out-of-pocket premium rose from $113 per month in 2025 to $178 per month in 2026, according to the CMS report.
- There are also more enrollees in “bronze” plans with higher deductibles this year: 40% of enrollees compared with 30% last year.
- Larry Levitt, executive vice president of health policy at KFF, wrote on X that the average premium increase would have been higher if some people had not switched into bronze plans with higher deductibles to try to keep their premiums down.
The big picture: 23.1 million people signed up for 2026 coverage, down 1.2 million from 2025.
- CMS touted its enforcement actions, which it said removed coverage or subsidies from nearly 1.5 million people found to be ineligible.