Shaler couple faces new charges over $30K in unpaid ambulance bills
This action highlights a longstanding problem in ambulance reimbursement: when insurers send payment directly to patients rather than the provider that delivered the care, everyone loses.
While these cases are relatively uncommon, they underscore why 𝐝𝐢𝐫𝐞𝐜𝐭 𝐩𝐚𝐲𝐦𝐞𝐧𝐭 𝐥𝐞𝐠𝐢𝐬𝐥𝐚𝐭𝐢𝐨𝐧, 𝐥𝐢𝐤𝐞 𝐭𝐡𝐞 𝐨𝐧𝐞 𝐢𝐧 𝐏𝐀 𝐫𝐞𝐟𝐞𝐫𝐞𝐧𝐜𝐞𝐝 𝐢𝐧 𝐭𝐡𝐞 𝐧𝐞𝐰𝐬 𝐫𝐞𝐩𝐨𝐫𝐭, 𝐢𝐬 𝐬𝐨 𝐢𝐦𝐩𝐨𝐫𝐭𝐚𝐧𝐭. Requiring insurers to pay ambulance providers directly ensures that reimbursement reaches the organization that incurred the cost of readiness, staffing, vehicles, and patient care.
It also protects patients from inadvertently becoming entangled in billing disputes, collection actions, or even criminal allegations when insurance checks are misused or misunderstood.
Direct payment laws create a simpler, more transparent process that supports the financial sustainability of EMS agencies while reducing confusion and stress for the very patients these systems are designed to serve.
PWW Advisory Group 𝐡𝐚𝐬 𝐝𝐞𝐯𝐞𝐥𝐨𝐩𝐞𝐝 𝐚 𝐬𝐮𝐦𝐦𝐚𝐫𝐲 𝐰𝐢𝐭𝐡 𝐬𝐨𝐮𝐫𝐜𝐞 𝐝𝐨𝐜𝐮𝐦𝐞𝐧𝐭𝐬 𝐨𝐟 𝐬𝐭𝐚𝐭𝐞 𝐥𝐚𝐰𝐬 𝐚𝐝𝐝𝐫𝐞𝐬𝐬𝐢𝐧𝐠 𝐏𝐚𝐭𝐢𝐞𝐧𝐭 𝐏𝐫𝐨𝐭𝐞𝐜𝐭𝐢𝐨𝐧/𝐁𝐚𝐥𝐚𝐧𝐜𝐞 𝐁𝐢𝐥𝐥𝐢𝐧𝐠, 𝐦𝐚𝐧𝐲 𝐨𝐟 𝐰𝐡𝐢𝐜𝐡 𝐢𝐧𝐜𝐥𝐮𝐝𝐞 𝐝𝐢𝐫𝐞𝐜𝐭 𝐩𝐚𝐲 𝐩𝐫𝐨𝐯𝐢𝐬𝐢𝐨𝐧𝐬. 𝐂𝐥𝐢𝐜𝐤 𝐡𝐞𝐫𝐞 𝐭𝐨 𝐯𝐢𝐞𝐰 𝐚𝐧𝐝 𝐝𝐨𝐰𝐧𝐥𝐨𝐚𝐝 𝐭𝐡𝐞 𝐬𝐮𝐦𝐦𝐚𝐫𝐲: https://www.pwwag.com/resources/summary-state-patient-protection-balance-billing-laws
Shaler couple faces new charges over $30K in unpaid ambulance bills
Shaler Hampton EMS took Stacie Hodge to various hospitals 23 times in about one year, director says
By Brian C. Rittmeyer
June 8, 2026
A Shaler couple facing criminal charges for not paying ambulance bills from Ross/West View EMS also owes more than $30,000 to Shaler Hampton EMS, according to additional charges filed against them.
Shaler Hampton EMS Director Eric Schmidt said it is reflective of a bigger issue that cost his agency just over $150,000 in 2025 — and one that proposed state legislation is intended to fix.
Shaler police filed charges June 4 against Wallace Hodge, 57, and Stacie Hodge, 43, the day after Ross police charged the couple.
Ross police allege the Hodges received nearly $8,000 from their insurer, Highmark, to pay Ross/West View EMS for six ambulance trips to hospitals, five from March to December 2025 and one in January, but did not pay those bills.
According to a criminal complaint, Schmidt told Shaler police that Stacie Hodge had been taken to various hospitals 23 times between Feb. 18, 2025, and Feb. 7, 2026, and had not paid for those services.
Shaler Hampton EMS billed Stacie Hodge’s insurer, Highmark. But because Shaler Hampton EMS does not have a contract with Highmark, the checks from Highmark were issued to Stacie Hodge with a message stating the EMS service is out of network and to forward the check to them, the complaint states.
Stacie Hodge did not forward the money to Shaler Hampton EMS, according to the complaint.
A search warrant for the couple’s checking accounts found that the Highmark checks to Stacie Hodge were endorsed by each of them and deposited into Wallace Hodge’s accounts.
According to the complaint, Shaler Hampton EMS billed Stacie Hodge $33,791.20. She had made payments totaling $2,193.44, leaving $30,710 owed.
In the complaint, Shaler police said they spoke with Wallace Hodge on Feb. 16. He said his wife was recovering from surgery at Allegheny General Hospital and participating in a study for ongoing seizures.
While police told Wallace Hodge they wanted to speak with his wife, neither of them have since contacted police, the complaint states.
According to the complaint, the Hodges told Schmidt that they used the money from Highmark for bills and other purchases. Stacie Hodge commented about having an expensive car payment and home expenses.
Part of a bigger issue, director says
While Schmidt told TribLive that the alleged case of the Hodges is “extreme,” it is only part of a problem.
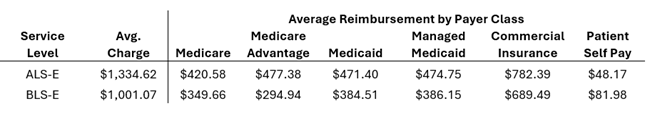
In 2025, 105 out of 233 patients with Highmark insurance, about 45%, kept the money they were given to pay Shaler Hampton EMS, accounting for $150,000 of the $333,740 charged.
Conversely, out of 250 patients with UPMC insurance, only three did not pay, totaling just over $4,000 out of just over $336,000 charged, according to data provided by Schmidt.
The difference is that UPMC sends payments directly to Shaler Hampton EMS, Schmidt said. Because his agency is not under contract with Highmark, it sends payments to patients.
“Highmark is the only company that does that in this market,” he said.
Schmidt said Shaler Hampton EMS, and all EMS agencies in Allegheny County, are not under contract with Highmark because they would then be reimbursed less than providing the service costs.
The money that Shaler Hampton EMS is owed could be used to buy lifesaving equipment and deal with the rising costs of fuel, Schmidt said.
Highmark spokesman Aaron Billger said the insurer does not make direct payment to out-of-network providers, including EMS agencies.
“Our first priority is to our members and clients,” he said. “Providing direct payment without contractual protections and without a tie to the amount of payment is simply not in the best interest of our members.”
Legislation proposed in the state General Assembly, and a concurring bill in the Senate, would mandate direct payment to EMS providers.
Senate Bill 1342, whose sponsors include state Sen. Devlin Robinson, R-Bridgeville, is a companion measure to House Bill 1152, whose backers include state Reps. Jill Cooper, R-Murrysville, and Arvind Venkat, D-McCandless.
They would require insurers to provide “fair and direct” reimbursement for mandated 911 emergency medical services regardless of whether the EMS provider is in network.
“Our EMS providers are facing an ongoing financial crisis while continuing to answer every emergency call, every hour of every day,” Robinson said. “These professionals do not have the option to decline service based on reimbursement rates or insurance status. This legislation recognizes the essential nature of emergency medical services and helps provide the financial stability needed to keep ambulances on the road and providers serving our communities.”
Cooper says her measure has strong bipartisan support, with 68 cosponsors.
”My legislation puts a circle around 911 calls because that is what every municipality and ambulance in the state is required by law to make that call. They can’t say, ‘Oh, no, we’re not coming,’ ” she said. “The reason for this bill is to help sustain our ambulance services so they can receive the payment directly from the insurance company so they’re not spending time chasing payments.”
The Hodges do not have attorneys listed in court records.
Shaler police charged Wallace Hodge with felony counts of theft of services, theft by failure to make required disposition of funds received and conspiracy. Stacie Hodge also is charged with felony counts of theft by failure to make required disposition of funds received and conspiracy, and a misdemeanor count of theft of services, according to court records.
Ross police charged each of them with felony counts of theft by failure to make required disposition of funds and criminal conspiracy, and a misdemeanor count of theft of services.
They were arraigned June 5 on both sets of charges and released on nonmonetary bonds, according to court records.
Their preliminary hearings on the Ross charges are scheduled for June 24 before District Judge Richard G. Opiela. For the Shaler charges, their preliminary hearings are set for June 25 before District Judge Daniel J. Konieczka Jr.