EMSIntel Surpasses 4,000 Curated News Reports, Evolving from Weekly Briefing to National EMS Intelligence Platform
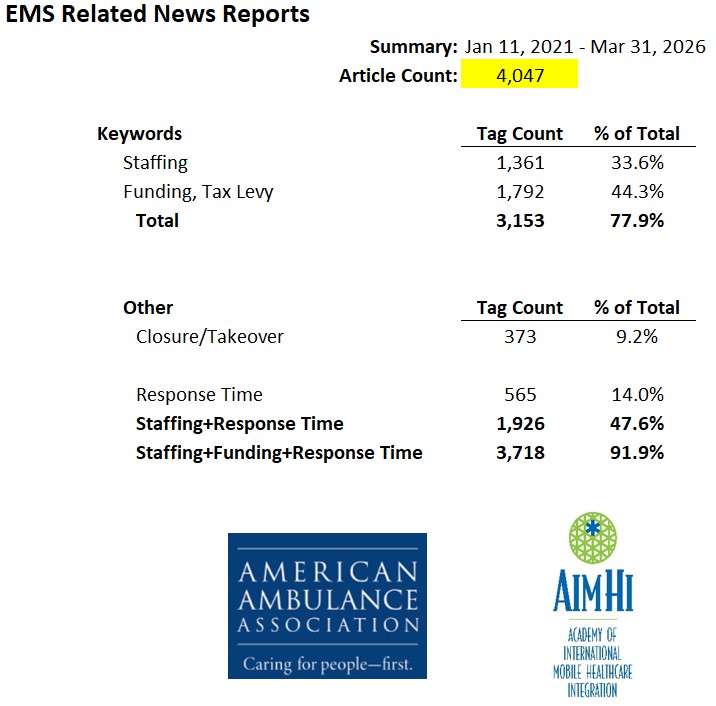
The go-to data base for conducting analysis of EMS trends ranging from finance and reimbursement to crashes and thefts – EMSIntel has now passed 4,000 news items and continues to grow.
What began as a simple weekly spreadsheet collated during the pandemic, tracking news reports about EMS, has grown into one of the most influential intelligence resources in Emergency Medical Services. EMSIntel, publicly accessible at www.emsintel.org, has surpassed 4,000 curated profession wide news stories, marking a significant milestone in its evolution from informal briefing tool to a nationally recognized platform for insight, analysis, and understanding.
The origins of EMSIntel are deliberately modest. Developed by Rob Lawrence (Pro EMS), while serving as the American Ambulance Association’s (AAA) Communications Chair, as a weekly compilation of notable EMS developments, the early version was shared with a small network of colleagues seeking clarity in an increasingly noisy information environment.
Recognizing both the value of the content and the opportunity to scale its impact, the AAA provided generous funding and support to transform EMSIntel from a static, spreadsheet-based product into the interactive and searchable platform it is today. This transition marked a pivotal moment, enabling not just collection, but structured collation and accessible analysis at scale.
As the platform matured, the Academy of International Mobile Healthcare Integration joined the collaboration, reinforcing EMSIntel’s role as a shared industry asset and ensuring its continued growth through coordinated collection, curation, and collaboration. Together, these partnerships have anchored EMSIntel firmly within the EMS ecosystem, both reflective of and responsive to its evolving needs.
From its earliest days, EMSIntel has been guided by a disciplined approach to curation and interpretation. Rodney Dyche (Patient Care EMS Solutions) serves as Chief Curator, overseeing the identification and classification of developments from across the United States and internationally. Matt Zavadsky (PWW|AG / Executive Director AIMHI) provides analytical leadership, translating thousands of individual entries into thematic insights that reveal the pressures, trends, and opportunities shaping EMS systems. Rob Lawrence shapes the input into briefings and articles to inform of issues, concerns and alerts.
An analytical summary of EMSIntel and a downloadable Excel file of the EMSIntel log, complete with source references, is updated each month on AIMHI’s News site.
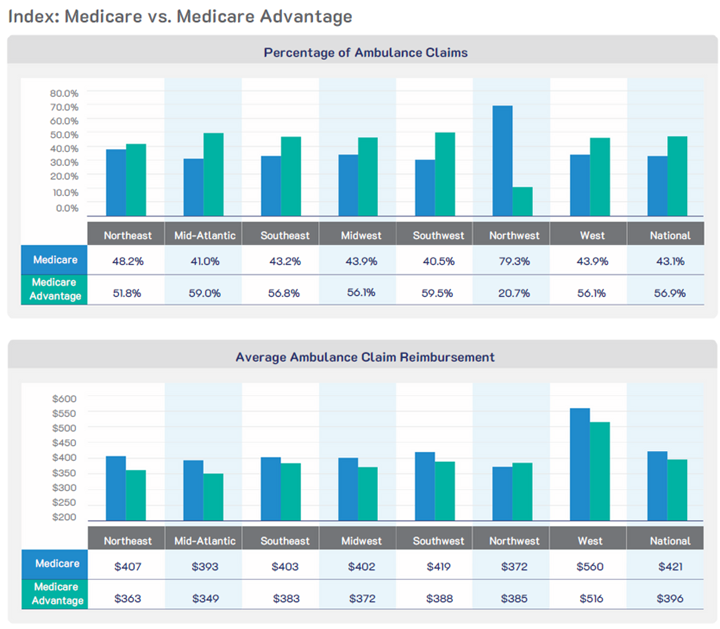
This structure and support allows EMSIntel to move decisively beyond aggregation. With more than 4,000 curated entries, the platform now supports meaningful thematic analysis across workforce challenges, reimbursement reform, ambulance patient offload times (APOT), mobile integrated healthcare, and system resilience. It offers not just a snapshot of events, but a longitudinal understanding of how the EMS landscape is changing.
That insight is increasingly being put to use. EMSIntel analysis has supported briefings for policymakers at both state and federal levels, providing evidence and context to inform legislative and regulatory discussions. It has also been cited in journalistic reporting, helping frame EMS issues within a broader, data-informed narrative.
“EMS has no shortage of information, but it often lacks shared understanding,” said Rob Lawrence. “EMSIntel was created to bridge that gap, turning noise into insight, and insight into something that can inform decisions, policy, and public awareness.”
As EMSIntel enters its next phase, the focus will remain on expanding its analytical capability while maintaining the disciplined curation that underpins its value. The milestone of 4,000 entries is not simply a measure of scale, but a signal that EMS now has a growing intelligence function, one capable of tracking, interpreting, and communicating the realities of a complex and evolving system.
About www.EMSIntel.org
EMSIntel is a curated intelligence platform focused on tracking and analyzing developments across the Emergency Medical Services sector. Created by Rob Lawrence and supported by Chief Curator Rodney Dyche and Analyst Matt Zavadsky. EMSIntel provides thematic insight into emerging trends and issues affecting EMS systems, policy, and practice. Learn more at www.emsintel.org
Published analysis derived from EMS Intel
Leading into 2026: The four actions every EMS leader must take: Leading into 2026: The four actions every EMS leader must take
EMS at the edge: Inside a year of reckoning and redesign: EMS at the edge: Inside a year of reckoning and redesign
Funding on fire: Communities are saying the quiet part out loud: Rethinking EMS funding: New models for ambulance service sustainability
Fast & spurious: America keeps losing ambulances and the fix is cheap: Prevent ambulance thefts: Keep paramedics, patients and the public safe